On August 24, 1960, two-year-old Greg Wallace sat in a waiting room at VGH with his mother, Doreen. At the time, the young boy couldn’t have known what was about to happen. His mother carried that burden, but knew it was the best option for her son. After all, ever since Greg was born he cried all the time, and was lethargic and tired. Not spritely, like the other children.
Greg would soon be gently placed under anaesthesia and wheeled on a gurney into an operating room at VGH, where he would undergo open-heart surgery by Dr. Philip Ashmore.
Greg had the misfortune of being born with ASD, or atrial septal defect, which means he had a hole in his heart between the upper chambers (the atria). The hole increases the amount of blood that flows through the lungs, and a large, long-term ASD can damage the heart and lungs, and in extreme cases cause complications such as arrythmias, stroke, and even early death.
Yet thanks to the then cutting-edge surgeons, Greg’s heart was surgically restored and his life was saved.
Did You Know?
VGH performs over 5,000 minimally-invasive cardiac procedures using a catheter each year.
Decades of heart health advancement
In 1960, Greg’s open-heart surgery for his ASD was the best option available. Although it did save his life, Greg would go on to suffer complications and a reduced quality of life. By age seven, Greg weighed 39 pounds and was quite frail.

“As a young man from Kamloops in love with hockey, I had to come to terms with a lot of what I could and could not do,” says Greg.
Although Greg’s life was saved, treatments nowadays for ASD and other heart conditions have greatly improved. Thanks to astounding medical advancements—often made possible due to philanthropic funding—an ASD repair would more often be treated with minimally invasive surgery over open-heart. This means better recoveries and better outcomes.

The fact is, many conditions which would have required invasive surgeries, followed by months if not years of recovery, have been turned into the most minimally invasive version surgeons can offer. An example of that would be structural heart disease, where now surgeons are able to replace heart valves in the morning and have patients go back home in the evening.
Transcatheter Aortic Valve Replacement (TAVR)
Widely considered one of the most exciting events in cardiology in decades, Dr. David Wood, Head of the Division of Cardiology at VGH, and Director of the Centre for Cardiovascular Innovation has standardized the minimally invasive heart valve replacement technique known as TAVR. This surgical procedure allows patients to have a transcatheter aortic valve replacement completed in the morning, and to be sent home by the evening. Prior to this technique, patients experienced open-heart surgery followed by months of challenging recovery.

Structural heart disease, coronary heart rhythm management, heart failure, women’s heart health, and more are all advancing on a global level right here in Vancouver. And thanks to these advancements, many people will not only survive like Greg, but go on to thrive.
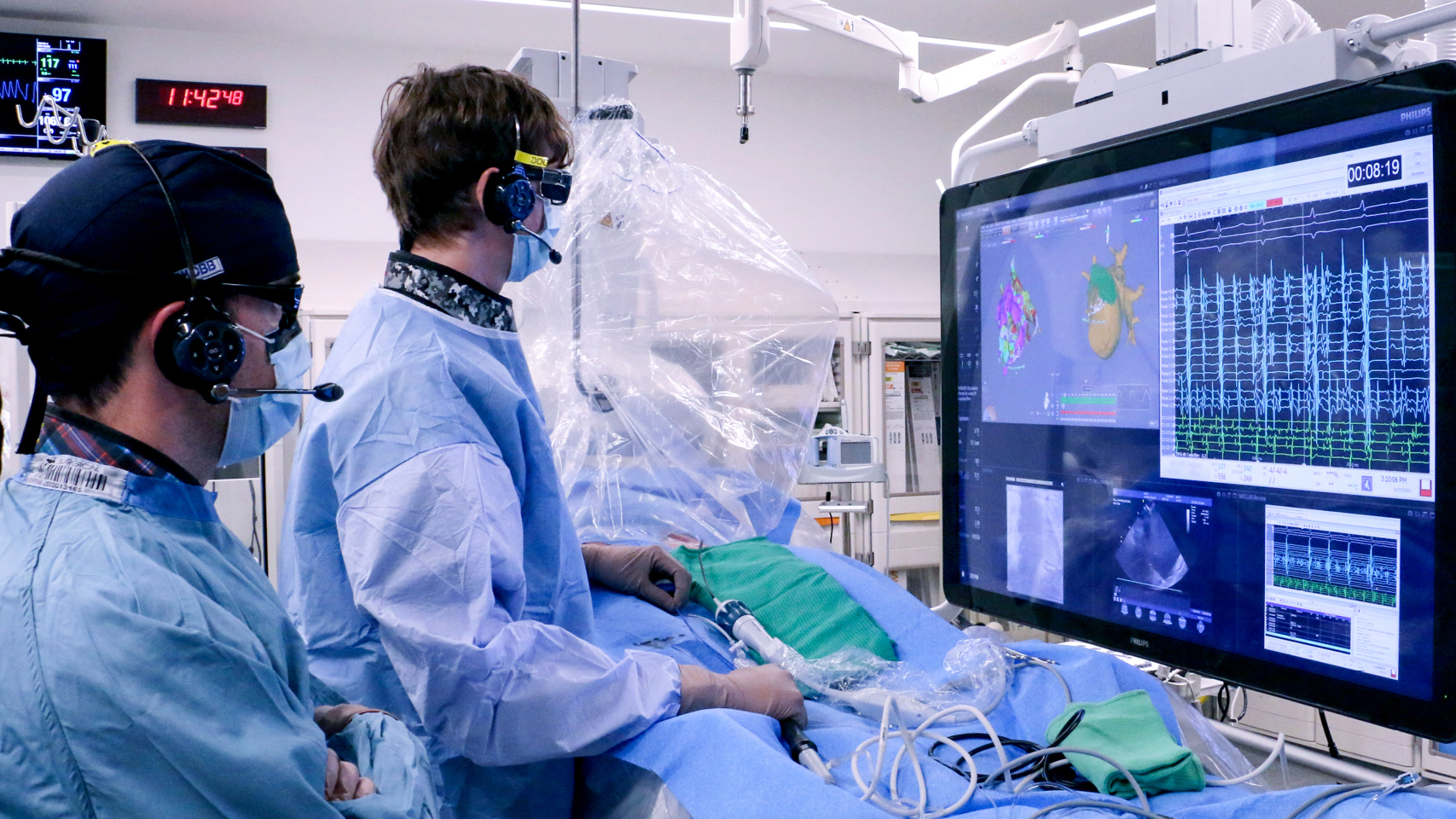
Electrophysiology Lab
At VGH, the electrophysiology (EP) laboratory empowers clinician-scientists to provide the most advanced care for complex cardiac conditions and diseases in Canada. This donor-funded, state-of-the-art space is equipped with a fluoroscopy machine for x-rays and a three-dimensional computer mapping system, allowing physicians to map the heart and determine where an arrythmia is situated.
Greg didn’t get a chance to play hockey, but he did have a successful career as the Kamloops Blazers Junior Hockey Clubs’ trainer and equipment manager from 1984 to 2007. He was inducted into the Kamloops Sports Hall of Fame and just recently his name was raised to the rafters in the Kamloops Blazers ‘Legends’ program.
“I wish I could have had the treatments they offer now,” says Greg. “But, I am incredibly grateful for the gift I was given as a child.”
Share this: